The observation of granulocyte adherence to the venous endothelium, lymphocyte infiltration and enhanced chemokine expression in the walls of varicose veins suggest an inflammatory process activated by bacteria. This is because these findings are difficult to explain as the sole consequence of destructive physical factors like elevated venous pressure.
WALDEMAR L. OLSZEWSKI We searched for bacteria using specimens obtained during routine varicose vein surgery. After thorough skin cleansing fragments of vein were excised and placed in culture medium. Other fragments of the same vein and adjacent tissues (fat and muscle) were placed on Hemoline® plates and cultured for 7 – 28 days at 37oC. Bacteria migrating from the tissue formed colonies which were characterized under the microscope. The on-plate culture method allowed optical evaluation of migration activity of different strains, density of colonies and competition between strains. Comparisons between bacterial strains growing on the Hemoline plate were made with those from liquid media.
Varicose veins specimens cultured in fluid media revealed the presence of bacterial isolates in 40%, whereas controls taken from healthy cadaveric organ donors contained live bacteria in only 4%. Disinfected skin specimens taken from phlebectomy sites showed the presence of microbes in 4%. The dominant isolates from vein specimens were Staphylococci, predominately coagulase negative. In a few cases, Enterococcus faecium was also detected. The Staphylococci were highly sensitive to most antibiotics, except penicillin. Thirty-three percent of isolates were methicillin resistant (MRSA). Interestingly, the Hemoline plates revealed microbes migrating from the varices and adjacent fat but not from the muscles (92% of specimens).
The high prevalence of isolates in the walls of varicose veins as well as the pictures of bacteria migrating out from the specimens after long-term culture are strong evidence for the pre-existence of bacteria in these tissues. However, it remains unknown whether these bacteria play a role in the pathogenesis of varicose veins. They may be an additional destructive factor and predispose to local thrombosis and, in certain cases, to the development of ulcers.
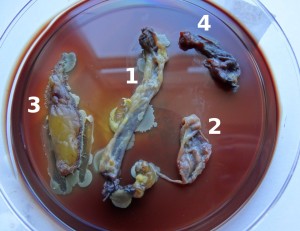 Fragments of vein outer wall (1), vein intima (2), perivenous tissue (3) and muscle (4), explanted on Hemoline® plates.
Fragments of vein outer wall (1), vein intima (2), perivenous tissue (3) and muscle (4), explanted on Hemoline® plates.