Cannulation is always painful and uncomfortable to the extent it may result in the development of needle phobias in some patients. Current developments to reduce pain include the application of local anaesthetic cream, smaller needles and nearby pressure to dampen and modulate the pricking sensation. With multiple needle punctures, such as that occurring during phlebectomies or tumescent anaesthesia, a way of reducing pain may make many local anaesthetic procedures more patient friendly. Vibrating needles are a promising development. The optimal vibrating frequency and direction of vibration, lateral or back & forth (like the mosquito), requires more research.
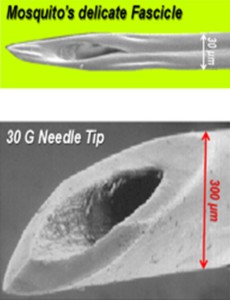
JOHN MARX The basic design of the hypodermic needle has essentially remained unchanged for the past 150 years. Hypodermic needles to cannulate veins cause pain during skin puncture. A needle has been developed which reduces the pain significantly and has greater precision at targeting the vein. It relies on the principle of vibration to cut its way through the tissues in a similar way that mimics the mosquito. Penetration force is reduced and there is less likelihood of the needle becoming stuck or overshooting the target.
The modern hypodermic needle is impaired by 2 major physical problems: penetration resistance and stiction. Stiction or “static friction” is the threshold force required to enable stationary objects in contact to move relative to one another. The addition of a vibration component to a hypodermic needle has been shown to reduce penetration resistance by 57% and stiction by 36%.
A device like the Marksman hypodermic is a “smart” needle because an optimum lateral vibration frequency can be calculated for each individual patient to achieve less pain with a greater ease of penetration and improved precision (less stiction). The variables which have been shown to affect performance include age, sex, skin type and needle gauge. These can be entered into the system to estimate the optimal vibration frequency.